|
We chose this route because continuous capnography is the earliest possible warning system for detecting the onset of opioid-induced respiratory depression (see " Spot the First Signs of Respiratory Compromise"). Both assumptions, in my estimation, are inaccurate.Īt the end of 2013, our organization started down the road toward making continuous capnography the standard of care for all adult and pediatric patients before, during and after procedural sedation or surgical procedures. Others may resist adding another monitoring tool to the mix, because they believe doing so would create additional work without significant payoff. 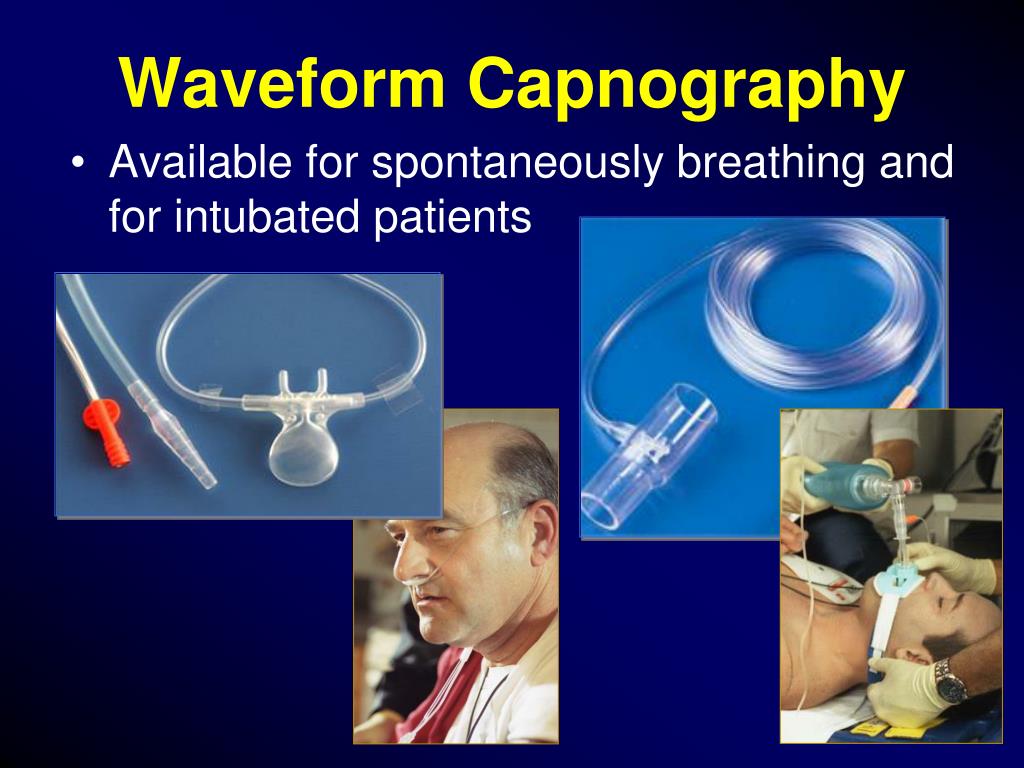
In addition, some clinicians may feel confident that monitoring other vital signs - blood pressure, body temperature, heart rate and blood oxygen levels - is sufficient. But I think improving patient outcomes and the potential for saving lives outweigh budgetary concerns. Why? Cost may be one barrier to adoption, as capnography can require a significant capital investment. With capnography, you find out in real time.ĭespite its superior ability to detect medication-induced respiratory events, capnography isn't as ubiquitous as other forms of vital signs monitoring. Also, after a shift in oxygen delivery, several minutes can elapse before a pulse oximeter provides an accurate reading, meaning the patient may already be in distress by the time you know it. As a result, turning up the oxygen would only mask the true nature of the problem. For example, if you see a troublesome oxygen saturation reading, you may simply choose to increase the oxygen flow without considering the potential causes for the change, such as a medication that might be relaxing the patient's airway. It still useful, but it also has its limitations. I began my healthcare career when pulse oximetry was considered a wonderful new monitoring tool. If the square becomes a flat line, the patient is not breathing. 
If the square waveform starts to collapse, there's an airway obstruction. If respiration decreases (hypoventilation), the waveform becomes taller and less frequent, and the numeric reading rises above the normal range. If the patient's respiratory rate increases (hyperventilation), the CO 2 waveform becomes smaller than the baseline and more frequent, and the numeric reading falls below the normal range. "Normal" end tidal CO 2 is in the range of 35 to 45 mmHg. On a capnography monitor, you see a real-time waveform (capnogram) - a normal waveform appears as a square-shaped or rectangular box - and a numeric reading (capnometry) showing the measurement of exhaled CO 2. Continuous capnography should be seen as a trending tool that provides a complete picture of a patient's ventilation, perfusion and metabolism. The word continuous is important, because a respiratory depression can occur when you're away from the patient's bedside. Nothing beats the close observation of expert nurses and anesthesia providers, but even your most attentive caregivers would benefit from being backed up by capnography.Ĭontinuous capnography is a breath-to-breath measurement of exhaled carbon dioxide at each phase of the respiratory cycle, gathered either through an advanced airway device (intubated) or a nasal cannula-type device (non-intubated). Without the monitoring modality, critical minutes may pass before you notice the patient is experiencing hypoventilation, airway obstruction or obstructive sleep apnea that could lead to respiratory arrest, cardiac arrest, hypoxic brain injury and even death. 
BIG PICTURE Continuous capnography offers a complete analysis of a patient's ventilation, perfusion and metabolism.Ĭapnography identifies potential respiratory events well before you have the sneaking suspicion that something seems amiss.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
